Less than half of gay and bisexual men have tested for HIV recently
The proportion of gay, bisexual and other men who have sex with men (GBM) reporting an HIV test is the highest ever recorded, according to findings from the 2014 Gay Auckland Periodic Sex Survey (GAPSS) and Gay men’s Online Sex Survey (GOSS) released before World AIDS Day on December 1.
Overall, 83 percent of GAPSS respondents and 70 percent of GOSS respondents had tested for HIV at least once in their lifetime. However often these tests happened a long time ago meaning less than half of all respondents had tested in the last 12 months.
“The gradual rise in lifetime testing coverage is very encouraging, but many gay and bisexual men aren’t testing as often as they need to, given their recent sexual behaviour,” says lead investigator Dr Peter Saxton from the Gay Men’s Sexual Health research group at the University of Auckland.
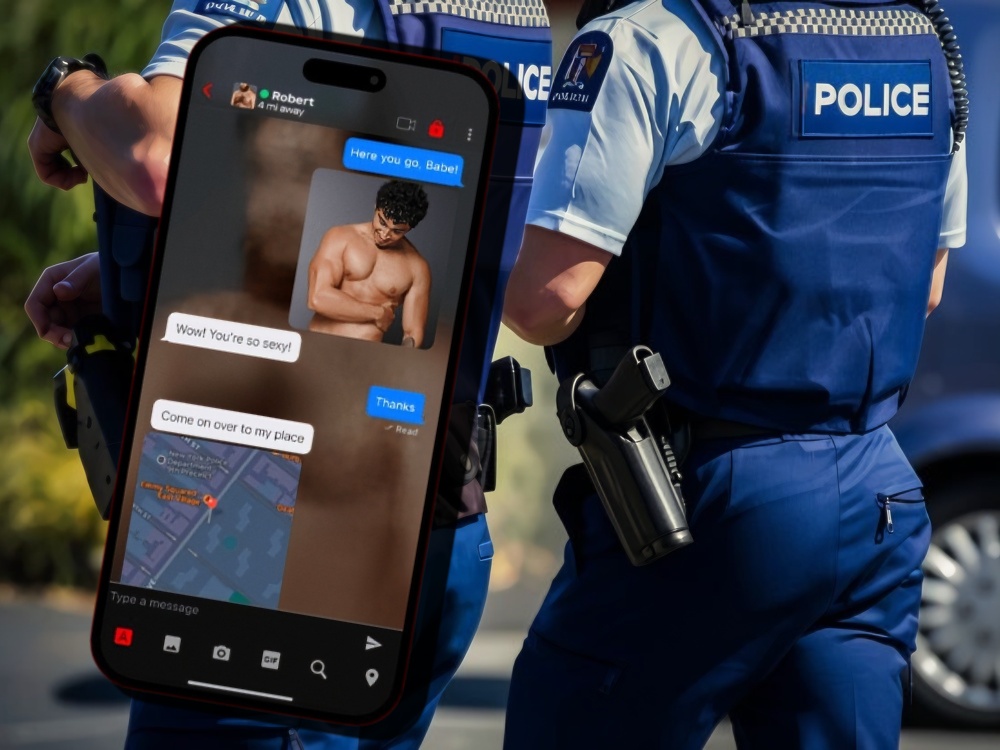
“Indicating that you’ve tested HIV negative is becoming an increasingly common sight on some online dating apps” says Dr Saxton, “but for some men this status will be outdated and ought to be described as ‘not sure’. We’d encourage men to think critically about when that last test was and what may have happened since then.”
Tony Hughes, co-investigator and NZAF Scientific Director says “unprotected anal intercourse since a last negative test may have resulted in a recently acquired undiagnosed HIV infection, which can be both asymptomatic and highly infectious.”
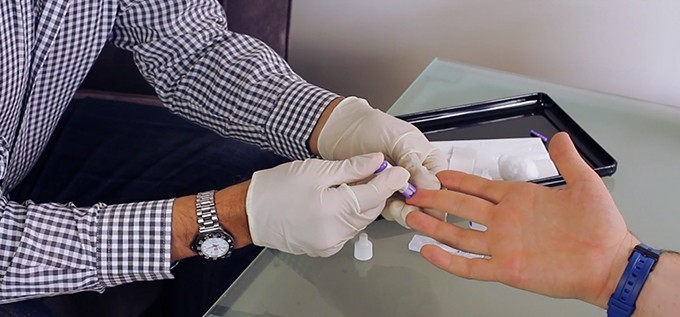
For the first time, as many men are choosing to test for HIV at sexual health clinics as at General Practices, and the popularity of rapid testing offered by NZAF and Body Positive also continues to rise.
The 2014 surveys recorded the highest ever proportion of diagnosed HIV positive respondents, at 6.2 percent of GAPSS participants and 4.1 percent of GOSS participants. This reflects ongoing infections in the gay community, increased testing and lower mortality due to treatments. Over three quarters of diagnosed positive respondents were currently on antiretroviral therapy.
Alongside condom use, HIV testing is a cornerstone of HIV prevention because individuals testing positive can be linked to antiretroviral treatment which improves wellbeing and reduces infectiousness to others.
“The key is a timely diagnosis” says co-investigator Associate Professor Nigel Dickson of the AIDS Epidemiology Group at the University of Otago. “A diagnosis soon after infection and before the immune system is seriously weakened gives a better outcome from treatment as well as limiting the possibility of further transmission.”
“Many people are still delaying testing” says Associate Professor Dickson. “In a 2011 study around one in five gay and bisexual men with HIV in Auckland were undiagnosed. Last year we found that over a third of the gay men diagnosed with HIV had low CD4 cell counts suggesting that they’d been living undiagnosed for several years.”
Gay and bisexual men are also increasingly optimistic about HIV because of new treatments, with 38% of all GAPSS participants in 2014 believing that HIV is a less serious threat than it used to be, compared to 20 percent reporting so in 2002.
Correspondingly, more respondents expected that gay men who know they have HIV would communicate their HIV status before sex happened, at around 40 percent of all participants in 2014.
“The rise in HIV disclosure expectations is interesting, because HIV positive individuals are often made to feel marginalised when they do disclose their status,” says Dr Saxton.
This year 3,214 respondents took part in GAPSS and GOSS. The studies have tracked behaviours and attitudes since 2002 and are jointly conducted by the University of Auckland, the University of Otago and the New Zealand AIDS Foundation with funding from the Ministry of Health.
Article | Levi Joule